Dr. Ramim Islam looks inside the surface. A medical officer specializing in internal medicine at Mymensingh Medical College Hospital (MMCH)- he can decipher the complexity of the interconnected anatomy, “All of the organ systems in the human body work synergistically. I look at it as a whole because a problem in one area can cause complications in another.”
Specialists who work in rural areas such as Dr. Ramim are essential to Bangladesh’s healthcare system. There are only 1.1 doctors per 10,000 population in rural areas, compared to 18.2 per 10,000 in urban areas. The intern doctor began his medical career in 2013, “I worked at the Upazila and Union level for two years. It was followed by a tenure at the indoor medical office in Rangpur Medical College for another two years before I joined my postgraduate studies with the Directorate General of Health Services (DGHS).”

Dr. Ramim’s academic career and field experience put him in a unique position during the pandemic. He is more equipped to handle the broad and comprehensive spectrum of illnesses that affect adults. Over 50% of infected COVID- 19 cases are among young adults (20-40 years old). “Internal medicine focuses on ailments that affect long term health in adults. We know the various types of tests that should be administered when a patient comes with a fever or a cough. These symptoms are not limited to COVID patients making it challenging to differentiate.” His training with the Strengthening Emergency Preparedness and Resilience in Bangladesh (SERB) program helped him prepare for the unique challenges that have arisen from the pandemic.
There is a Method to the Medicine
The One-Stop Service Center at MMCH has been running since 2017. It provides round the clock services for urgent medical care and timely treatment with over 40 diagnostic tests. Dr. Ramim recognizes the center as a means of controlling the outbreak by reducing the burden within the hospital- “The center provides treatment to patients that do not need to be admitted, lab facility to diagnose and short term treatment, and if the patient needs to be hospitalized. There is a 16-bed hospital room where in-patients can be treated one to two days for further diagnosis.”
The division has transformed into a flu corner during these times. Dr. Ramim observes that all hospitals with over 50 beds have provided treatment for both COVID and non-COVID patients. “A COVID-19 positive patient is transferred to the isolation center. The hospital consists of two buildings and we have dedicated three floors of the new building for COVID-19 treatment.” The hospital is understaffed like most healthcare institutions across Bangladesh. Every doctor, nurse, and technician has taken on the role of a COVID specialist.
Adopting Systemic Interventions
The indoor and outdoor facilities have made MMCH the primary hospital for COVID patients in the area. Patients with less complicated symptoms are treated outside in order to prevent increased chances of cross-infection. Dr. Ramim details the triage system established during the pandemic: “Patients without COVID-19 are sent for regular treatment with a green card. Those suspected of viral symptoms are sent to the flu corner with a yellow card. We admit patients with mild symptoms or those with serious conditions such as heart disease or diabetes.”
Minimizing interaction is essential to prevent the spread. Doctors from all backgrounds have been provided with a shortened guideline for COVID-19 which allows them to make a quick decision. Dr. Ramim links decisive action as crucial to stop the spread, “Medical officers that provide 24-hour service and there are senior physicians available for consulting via digital communication. We follow the national guidelines to divide patients according to mild, moderate, or severe symptoms.”
The institute has also divided the Intensive Care Unit (ICU) into a COVID-19 ICU section for patients whose conditions deteriorate despite oxygen therapy. The national ICU capacity is very limited- the entire public health system has 432 ICU beds, and only 110 are outside of the capital city Dhaka.
“The greatest limitation and challenge for medical institutes are the lack of manpower against the influx of patients,” observes Dr. Ramim. “The patient frequency has increased again with the loosening of the lockdown. Although 2,000 doctors have been recruited, it’s not sufficient on a national level.”
Operating with the Right Mindset
Dr. Ramim participated in the Hospital Preparedness for Emergencies (HOPE) course organized by the Asian Disaster Preparedness Center (ADPC) under USAID’s Strengthening Earthquake Resilience in Bangladesh (SERB) program in 2017. He gathers the mental strength to act because of the training: “Our work dynamics have changed into 24-day cycles. We work for 10 days and quarantine for two weeks before starting the next round.” Doctors must isolate away from their families as a necessary precautionary measure. The practice is necessary in Mymensingh where one out of 10 cases of COVID-19 cases are doctors.
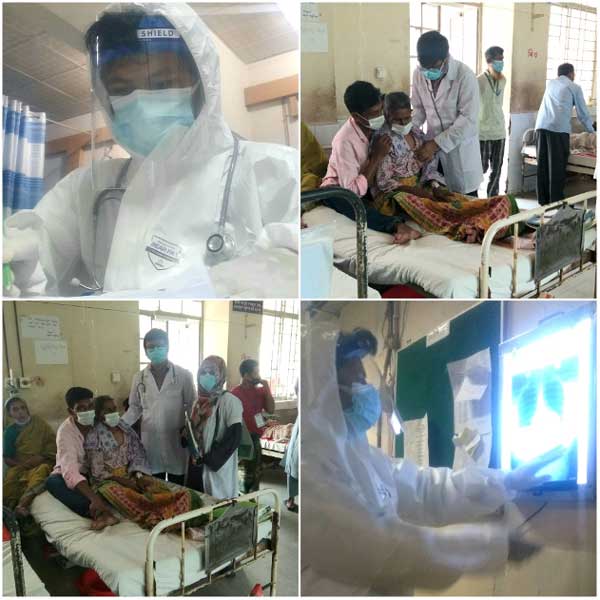
“The isolation can take a toll on our mental health. The training equipped me with the tools to power through and promote my own psychological well-being.” The doctor also recommends policymakers and medical practitioners alike because the knowledge can prevent the functional collapse of a hospital. “The simulation exercises are designed to comprehend and learn to act during an emergency situation in a time-sensitive manner. When we act in a strategic and proactive manner, we reduce the impact of a disaster.”
The HOPE course inspired the intern to attend the Training for Instructor (TFI) course. Dr. Ramim wanted to take on a more dynamic role in disaster preparedness. “My line of work requires a high state of alert. TFI has instilled a sense of planning that allows me to act methodically. When I realized we would not have enough PPE to treat patients- I immediately recommended that we purchase them ourselves because it is an investment in our own safety.” He is now able to facilitate meetings that foster a more cooperative effort with his peers. “The communication skills I gained have supported the ease of transactions with patients and authorities alike. TFI also stresses the importance of maintaining facilities through coordination with all personnel. The management skills are particularly essential during emergency and disaster situations when working modalities break their norm.” Under the SERB program, 22 HOPE and four TFI courses were conducted in the period from 2013 to 2019 in 12 cities in Bangladesh.
There are 11 major organs that facilitate breathing, eating, moving, and protecting humans from the outside environment. And none of them can work without the other. Dr. Ramin has taken this internist logic and applied it to his perspective of medicine, “The hospital needs to function as a healthy body because an institute that works together, heals together,”
The case study was developed under the South-South facility of the Asian Preparedness Partnership (APP) and SERB. At APP, we believe in amplifying voices that build upon South-South knowledge and learning exchange. Our platforms and initiatives are dedicated to supporting countries during COVID-19.
This document was made possible with the generous support of the American Peoplethrough the USAID Bureau of Humanitarian Assistance (USAID-BHA). Prepared by the Asian Disaster Preparedness Center (ADPC) for the SERB.
“Disclaimer – This study/report (Taking Medical Intern-ventions) is made possible by the support of the American People through the United States Agency for International Development (USAID). The contents and views of this document are the author’s and do not necessarily reflect the views of USAID or the United States Government.”



Comments are closed.